It’s one of the hardest conversations an eye doctor can have with a patient: “You’re going to become blind.”
But that’s the bottom line for retinitis pigmentosa (RP). The inherited eye disease is incurable. Symptoms typically first appear during childhood, but many people go blind by age 40.
Vision preservation a possibility
However, research by a UCI Health ophthalmologist has generated hope that a treatment to preserve vision may be within reach.
Dr. Henry Klassen, associate professor and director of the Stem Cell and Retinal Regeneration Program at UC Irvine School of Medicine, has launched a Phase 2b clinical trial to test the safety and efficacy of a stem cell therapy to stop the disease progression.
It’s a major step forward in an FDA-approved stem cell-based clinical study.
His research may have far-reaching impact as stem cell therapy offers a promising approach for a number of devastating diseases. Klassen’s research was accelerated by support for the state’s stem cell agency, the California Institute for Regenerative Medicine.
A two-decade search for treatment
The study is a high point in Klassen’s two-decade quest to find a treatment for RP. Even during medical school, he was intrigued with the idea that tissues in the central nervous system — the brain, spine, retina — could be coaxed into repair after damage.
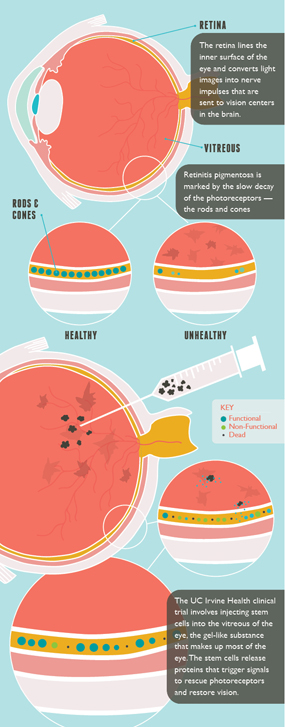
He focused on RP, which is caused by the deterioration of light-sensing cells in the eye called rods and cones.
“What was amazing about RP was how severe it is and yet how precise the lesion is. The fundamental problem is the rods and cones are going away,” says Klassen.
Eventually technology caught up with Klassen’s dream of developing an RP treatment. Late one night, while studying in Europe, Klassen received a call from a colleague who said he’d successfully implanted stem cells into the retina of a laboratory rat. Klassen hopped on a plane to see the research for himself. Stem cells are immature cells that can both divide and differentiate into other tissues.
“I took one look down the microscope, and it was so stunning and unexpected,” Klassen says. “I dropped everything and said, ‘This is what I’m going to work on.’ I was all in.”
Focusing on stem cells
The therapy now under investigation involves progenitor cells, which have begun the differentiation process from stem cells but are still immature, and were developed in Klassen’s lab at the UC Irvine Sue & Bill Gross Stem Cell Research Center.
His colleague, Dr. Jing Yang, prepares the cells from each patient and brings them to the treating physician.
At the Gavin Herbert Eye Institute, Dr. Barry Kuppermann injects the cells into the vitreous of the eye — the gel-like substance that makes up much of the inner eye — of RP patients.
The process is illustrated at left. Click the image to enlarge it.
Reversing retinitis pigmentosa?
Studies so far show that the stem cells secrete growth factors that rescue damaged retinal cells and slow disease progression. They may also prompt the growth of new rods and cones to replace dying retinal cells and possibly reverse the course of the disease.
“The initial goal was to slow the progression,” Klassen says.
“But we had to start the clinical testing in people who were already severely affected. We’re excited that some of the patients reported that they were getting better. That was more than we expected.”
RP affects 1.5 million people worldwide and is considered a rare, orphan disease. The Food and Drug Administration has granted Klassen and his colleagues a Regenerative Medicine Advanced Therapy designation, which allows for an expedited review of promising therapies.
Klassen, who ran the mile in track during high school, knows the final steps can be the most thrilling and the most taxing.
“We’ve come a long way,” he says. “We know that we have to get over the finish line.”
Related stories



